Recently, the 2026 report “Under the Weather: India’s Climate-Health Intersections and Pathways to Resilience” by ClimateRISE Alliance and Dasra (a philanthropy fund organisation) highlighted that nearly 40% of India’s districts are highly vulnerable, identifying climate change as a “health-risk multiplier” and an emerging core determinant of public health.
Best Online Coaching for UPSC
Key Highlights of the Report
The report underscores that climate change is a health-risk multiplier and inequality amplifier, necessitating a systemic, integrated, and resilience-oriented public health response.
- Climate Change as a Systemic Public Health & Development Crisis: The report clearly establishes climate change as a systemic, multi-sectoral crisis, extending beyond environmental concerns into public health, economic productivity, and social stability.
- It highlights the emergence of a climate–health–economy nexus, where environmental degradation directly leads to disease burden, reduced human capital, and developmental setbacks.
- This framing is reinforced by the World Health Organization, which identifies climate change as the most significant global health threat.
- Climate as a “Health-Risk Multiplier” & Epidemiological Transformer: The report underscores that climate change acts as a “health-risk multiplier”, intensifying pre-existing vulnerabilities rather than operating in isolation.
- It simultaneously increases communicable diseases (such as dengue and malaria), exacerbates non-communicable diseases (including cardiovascular and respiratory illnesses), and amplifies heat-related health risks.
- Additionally, it is reshaping disease geography, enabling vector-borne diseases to expand into previously unaffected regions, including hilly and temperate zones.
- According to the Lancet Countdown, there has been a significant rise in climatic suitability for dengue transmission in India.
- Patterns are for expanding the range of vector-borne diseases such as dengue and malaria into new regions.
- Areas that were previously unaffected, including Shimla, parts of Jammu & Kashmir, and the Himalayan foothills, are now reporting cases. The report also identifies Pune as a major dengue hotspot, with cases expected to rise further.
- Massive Economic & Productivity Losses: The report highlights that climate-induced health impacts are imposing severe macroeconomic costs, directly affecting labour productivity and national output.
- It notes that heat exposure led to the loss of nearly 160 billion labour hours in 2021, amounting to approximately 5.4% of India’s GDP.
- Heat stress reduces physical work capacity, particularly in labour-intensive sectors such as agriculture and construction, while also affecting urban productivity and cognitive performance.
- The International Labour Organization further projects that millions of jobs in India could be at risk due to rising heat stress by 2030.
- Chronic Health and Economic Burden of Air Pollution: Air pollution is identified as a persistent, slow-onset climate-linked health crisis, contributing significantly to mortality and economic losses.
- The report estimates that health impacts of air pollution cost India around 3% of its GDP annually, reflecting a substantial economic burden.
- It is strongly associated with respiratory illnesses, cardiovascular diseases, and premature mortality.
- The Indian Council of Medical Research estimates around 1.6 million deaths annually in India due to air pollution, while the World Bank highlights its impact on reducing life expectancy.
- Rising Heat Stress and Mortality Risks: The report establishes a clear correlation between increasing heatwaves and rising mortality rates, especially from cardiovascular conditions.
- It notes an approximately 11.7% increase in cardiovascular mortality risk during extreme heat events, along with rising cases of heatstroke, dehydration, and kidney-related disorders.
- Recent heatwave episodes in India (2023–24) have demonstrated sharp increases in hospitalisations and fatalities, particularly in northern and central regions.
- Climate Change as an Inequality Amplifier: The report emphasises that climate change disproportionately affects vulnerable populations, thereby acting as an inequality multiplier.
- Women, children, informal workers, and rural communities face higher exposure to climate risks and lower adaptive capacity.
- It also highlights that the crisis is not gender-neutral, with increased risks of maternal health complications and adverse birth outcomes under heat stress.
- The United Nations Children’s Fund notes that a large proportion of Indian children are highly vulnerable to climate-related risks.
- Systemic Gaps and the Need for an Integrated, Data-Driven Response: The report identifies critical structural gaps, including fragile healthcare systems, lack of granular climate-health data, and weak inter-sectoral coordination.
- It highlights a positive trend wherein nearly 70% of NGOs have integrated climate-health strategies since 2020, indicating a shift toward holistic approaches.
- It strongly advocates for:
- Climate-resilient healthcare infrastructure
- Localised, disaggregated data systems and AI-based surveillance
- Whole-of-society collaboration involving government, private sector, and civil society
- These recommendations align with the vision of National Institution for Transforming India, which emphasises integrated and resilience-oriented development pathways.
About Climate Change
- Refers: Climate Change refers to long-term alterations in global and regional climatic systems, primarily driven by anthropogenic Greenhouse Gas (GHG) emissions such as Carbon Dioxide (CO₂), Methane (CH₄), and Nitrous Oxide (N₂O).
- Observed Indicators: Climate change is evidenced through discernible alterations in Earth’s physical systems, including rising global and regional temperatures, increasing variability and unpredictability in precipitation patterns, accelerated glacier retreat, progressive sea-level rise, and a heightened frequency as well as intensity of extreme weather events such as heatwaves, floods, droughts, and cyclones.
- Scientific Consensus: The Intergovernmental Panel on Climate Change confirms that human activities have unequivocally warmed the atmosphere, ocean, and land, establishing climate change as a scientifically validated phenomenon.
Factors of Climate Change
- Anthropogenic Emissions and Pollution Drivers: Greenhouse Gas (GHG) emissions from fossil fuel combustion, industrialisation, and agriculture remain the primary structural drivers of climate change.
- Local pollution sources—including biomass burning, vehicular emissions, industrial discharge, and waste burning—create a climate–air pollution nexus, intensifying both global warming and health risks.
- Recent Evidence: India is among the top global emitters, and Particulate Matter (PM2.5) exposure linked to forest fires and pollution caused ~10,200 deaths annually (2020–2024).
- Urbanisation and Heat Amplification (Urban Heat Island Effect): Rapid urbanisation, concretisation, and shrinking green cover lead to the Urban Heat Island (UHI) effect, where cities experience significantly higher temperatures than surrounding areas.
- Urban structures trap heat and pollutants, intensifying heat stress and air pollution exposure.
- Example: Cities are warming nearly twice as fast as rural areas, and extreme rainfall and flooding in cities like Mumbai is linked to climate change and unplanned urbanisation.
- Informal Economy and Social Protection Deficit: A significant share of India’s workforce is in the informal sector, lacking:
- Health insurance and social security
- Income stability during climate shocks
- Climate-induced illnesses lead to high out-of-pocket expenditure, pushing households into poverty traps and debt cycles.
- This reflects a climate–poverty feedback loop, where vulnerability reinforces economic insecurity.
|
UPSC Online Classes
Impacts of Climate Change- A Multi-Dimensional Assessment
- Public Health Impacts- Climate as a Health-Risk Multiplier: Climate change represents the “lived experience of physiological and biological stress”, directly affecting human survival and well-being.
 It functions as a health-risk multiplier, as it intensifies pre-existing vulnerabilities such as poverty and malnutrition, accelerates disease transmission pathways, and overburdens already fragile healthcare systems.
It functions as a health-risk multiplier, as it intensifies pre-existing vulnerabilities such as poverty and malnutrition, accelerates disease transmission pathways, and overburdens already fragile healthcare systems.- It also undermines the fundamental determinants of health, including clean air, safe water, and stable food systems, thereby expanding the overall disease burden.
- The World Health Organization estimates that climate change could lead to approximately 250,000 additional deaths annually between 2030 and 2050, highlighting its scale as a public health crisis.
- Changing Disease Patterns and Epidemiological Shifts: Climate change is reshaping the geography and seasonality of diseases, leading to the expansion of vector-borne diseases such as dengue and malaria into previously non-endemic and high-altitude regions, including areas like Shimla and Jammu & Kashmir.
- It is also contributing to the emergence of new urban disease hotspots, with cities such as Pune witnessing rising dengue incidence due to microclimatic changes and urban water stagnation.
- Extreme weather events, particularly floods, trigger outbreaks of water-borne diseases such as cholera and hepatitis, especially in regions with inadequate sanitation and drainage infrastructure.
- The Indian Council of Medical Research has noted shifting disease patterns in India, underscoring the growing epidemiological challenge.
- Life-Course Impacts and Vulnerable Populations: Climate change exerts differential impacts across the human life cycle, with heightened vulnerability among women, children, and the elderly.
- Exposure to extreme heat and air pollution (Particulate Matter – PM2.5) is associated with adverse maternal outcomes, including hypertensive disorders such as pre-eclampsia, preterm births, and stillbirths.
- Infants and young children are particularly vulnerable due to their limited thermoregulatory capacity, making them more susceptible to heat stress, dehydration, and infections.
- Long-term exposure to polluted environments is linked to low birth weight, impaired lung development, asthma, and reduced overall health outcomes, reflecting intergenerational consequences of climate change.
- Gendered and Structural Inequalities: Climate change is not gender-neutral, as women face:
- Higher exposure due to livelihood roles
- Limited mobility and decision-making power
- Maternal and reproductive health risks (e.g., heat-linked preterm births)
- It disproportionately affects poor households, children, elderly, and coastal communities
- Example: Climate impacts interact with pre-existing socio-economic inequalities, leading to higher exposure but lower adaptive capacity.
- Those contributing least to emissions face the highest burden, highlighting climate justice concerns.
- Non-Communicable Diseases and Physiological Stress: Rising temperatures and environmental stressors are contributing to a significant increase in Non-Communicable Diseases (NCDs), particularly cardiovascular and respiratory conditions.
- Heat exposure imposes chronic cardiovascular stress, increasing the incidence of heart diseases and heat-related mortality.
- Climate-linked air pollution is a major driver of respiratory illnesses such as asthma and Chronic Obstructive Pulmonary Disease (COPD).
- Additionally, reduced safe windows for outdoor physical activity are contributing to physical inactivity and lifestyle-related diseases, as highlighted by the Lancet Countdown.
- Economic and Developmental Impacts: Climate change has emerged as a systemic developmental and economic risk, affecting productivity, livelihoods, and long-term growth trajectories.
- Heat stress significantly reduces labour productivity, particularly in climate-exposed sectors such as agriculture and construction, leading to loss of working hours and income.
- It also disrupts agricultural production and water availability, thereby affecting food security and nutritional outcomes.
- The National Institution for Transforming India highlights that climate variability is already adversely impacting agriculture, water resources, and rural livelihoods in India.
- Extreme Events, Infrastructure and Supply Chain Disruptions: Climate change is increasing the frequency, intensity, and unpredictability of extreme weather events, including heatwaves, floods, droughts, and cyclones.
- These events expose critical infrastructure vulnerabilities, particularly:
- Healthcare systems, which face service disruptions
- Transport and connectivity networks, which hinder emergency response
- Extreme weather also disrupts medical supply chains, including the availability of medicines, vaccines, and cold-chain logistics, thereby converting manageable health conditions into large-scale emergencies.
- Inequality, Climate Justice and Governance Challenges: Climate change acts as an inequality multiplier, disproportionately affecting women, children, elderly populations, informal workers, and economically weaker regions.
- These groups face higher exposure to climate risks but possess lower adaptive capacity, leading to deepening socio-economic disparities.
- The United Nations Development Programme highlights that populations contributing least to global emissions bear the greatest burden of climate impacts, raising critical concerns of climate justice.
- Addressing these challenges requires a paradigm shift in governance, moving from:
- Reactive to anticipatory approaches
- Curative to preventive and resilience-based public health systems
- India’s Heat Action Plans, supported by India Meteorological Department and National Disaster Management Authority, exemplify early warning-based adaptive governance frameworks.
Click to Know UPSC Offline Courses
Significance of Climate–Health Integration
- Economic Stability and Productivity Imperative: Addressing climate change is essential to safeguard economic productivity and national growth, as heat stress, disease burden, and environmental degradation directly reduce labour efficiency and workforce participation.
- Protecting population health is therefore integral to protecting Gross Domestic Product (GDP) and long-term economic capacity, particularly in climate-sensitive sectors such as agriculture and informal labour.
- Public Health Security and Human Survival: Climate change has emerged as a major public health threat, necessitating the integration of health considerations into climate policy frameworks.
- The World Health Organization emphasizes that placing health at the centre of climate action is critical to preventing large-scale mortality and disease burden.
- Without such integration, climate impacts risk overwhelming already stretched healthcare systems, especially in developing countries.
- Breaking the Climate–Poverty–Vulnerability Cycle: Climate change creates a self-reinforcing cycle of vulnerability, where:
- Loss of income due to climate shocks
- Rising healthcare expenditure push households into chronic poverty and indebtedness
- Integrated climate–health action is necessary to break this cycle and prevent intergenerational poverty traps, particularly among vulnerable populations.
- Environmental Justice and Equity Considerations: Climate change is fundamentally an issue of equity and justice, as those contributing least to emissions often bear the greatest impacts.
- The United Nations Development Programme highlights that addressing climate–health intersections is crucial to reducing socio-economic inequalities and protecting marginalised communities.
- Integrating health into climate policy ensures a people-centric and inclusive development approach.
- Co-Benefits of Integrated Climate Action: Climate–health integration generates multiple co-benefits, including:
- Improved health outcomes (reduced pollution-related diseases)
- Enhanced community resilience
- Increased economic productivity
- For example, clean energy transitions reduce emissions while simultaneously improving air quality and reducing disease burden, demonstrating synergistic policy gains.
- Strengthening Disaster Preparedness and Adaptive Capacity: Integrating health into climate policy enhances preparedness for climate-induced disasters, such as heatwaves, floods, and disease outbreaks.
- Early warning systems and adaptive strategies, such as Heat Action Plans supported by India Meteorological Department and National Disaster Management Authority, demonstrate the importance of anticipatory governance.
- Such measures reduce mortality, morbidity, and systemic disruption during extreme events.
- Long-Term Developmental Resilience: Climate change poses a significant risk to hard-earned developmental gains, particularly in areas such as health, poverty reduction, and food security.
- Building climate-resilient health systems is essential to ensure that development progress is sustained and not reversed by recurrent climate shocks.
- It enables a transition toward sustainable, resilient, and future-ready development pathways.
Challenges & Concerns in Tackling Climate Change (Climate–Health Context)
- Data Deficits and Evidence Gaps: A major constraint is the lack of granular, localised, and disaggregated data linking climate variables with specific health outcomes, which limits evidence-based policymaking.
- The absence of real-time surveillance and integrated climate–health databases restricts the ability to predict disease outbreaks and design targeted interventions.
- Skewed Climate Finance and Underfunded Adaptation: Climate finance remains disproportionately skewed toward mitigation efforts (such as renewable energy), while adaptation—particularly health system resilience—remains underfunded.
- This imbalance weakens the capacity to prepare for and respond to climate-induced health risks, especially in vulnerable regions.
- Fragmented Institutional and Governance Frameworks: Climate and health responses are often siloed across multiple ministries and agencies, resulting in:
- Poor coordination during disasters
- Duplication of efforts and policy gaps
- The absence of an integrated, cross-sectoral governance mechanism hampers efficient crisis response and long-term planning.
- Weak Public Awareness and Risk Perception: There is limited public awareness regarding the long-term health impacts of climate change, particularly:
- Chronic heat exposure
- Air pollution-related diseases
- This leads to low adoption of preventive behaviours and undermines community-level resilience and preparedness.
- Barriers to Grassroots and Community-Level Action: Local organisations and community-based institutions, especially in highly vulnerable regions, face:
- Limited access to climate finance
- Administrative and procedural hurdles
- This restricts context-specific, bottom-up adaptation strategies, which are critical for effective resilience building.
- Infrastructure Fragility and Health System Vulnerability: A large proportion of healthcare infrastructure is not climate-resilient, making it vulnerable to:
- Floods, cyclones, and extreme weather events
- This results in:
- Disruption of essential health services
- Collapse of care delivery during emergencies
- Systemic Inequality and Capacity Constraints: Climate change impacts are unevenly distributed, with vulnerable populations having:
- Higher exposure to risks
- Lower adaptive capacity
- Weak institutional capacity at local levels further limits implementation of climate–health policies, exacerbating existing socio-economic inequalities.
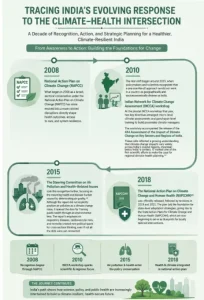
Actions & Initiatives Taken by India
- Policy Evolution and Institutional Framework:
- From Broad Climate Policy to Health Integration: India’s climate policy has evolved from broad environmental frameworks to health-centric approaches, recognising climate change as a public health challenge.
- The National Action Plan on Climate Change (NAPCC) provides the overarching strategy, while the National Action Plan on Climate Change and Human Health (NAPCCHH) marks a significant shift toward integrating health into climate governance.
- This reflects a transition from sectoral policies to a more integrated climate–health framework.
- Climate-Resilient Health Systems and Surveillance:
- National Programme on Climate Change and Human Health (NPCCHH): The NPCCHH, under the Ministry of Health and Family Welfare, focuses on:
- Capacity building of healthcare professionals
- Strengthening climate-sensitive disease surveillance
 Mainstreaming climate concerns into public health planning
Mainstreaming climate concerns into public health planning
- Digital Disease Surveillance: Programs such as the Integrated Disease Surveillance Programme (IDSP) leverage digital platforms for real-time monitoring of outbreaks, enabling early detection and rapid response to climate-sensitive diseases.
- Localised Adaptation and Heat Action Plans:
- Heat Action Plans (HAPs): India has implemented Heat Action Plans (HAPs) across multiple cities and states to reduce heat-related mortality and morbidity.
- These include:
- Early warning systems
- Public awareness campaigns
- Inter-agency coordination
- Supported by India Meteorological Department and National Disaster Management Authority, HAPs demonstrate localised, anticipatory climate governance.
 Decentralised and Community-Based Healthcare Delivery:
Decentralised and Community-Based Healthcare Delivery: -
- Strengthening Last-Mile Health Systems: India is increasingly focusing on decentralised healthcare delivery, bringing services closer to communities, particularly in climate-vulnerable regions.
- This reduces dependence on transport systems, which are often disrupted during climate disasters.
- Community-Level Adaptation: Public health outreach and community awareness initiatives are being strengthened to improve local resilience and adaptive capacity.
- Clean Energy Transition and Environmental Health Co-Benefits:
- Renewable Energy Expansion: India is advancing solar, wind, and green hydrogen initiatives under missions such as the National Solar Mission, contributing to reduced Greenhouse Gas (GHG) emissions.
- Air Quality Improvement: The National Clean Air Programme (NCAP) aims to reduce Particulate Matter (PM2.5 and PM10) levels, generating co-benefits for both climate mitigation and public health improvement.
- Innovation, Technology and Multi-Stakeholder Engagement:
- NGO and Private Sector Innovations: Civil society organisations are introducing:
- Solar-powered health facilities
- Artificial Intelligence (AI)-based disease tracking systems
- These innovations enhance adaptive capacity and service delivery in remote and vulnerable areas.
- Collaborative Platforms: Initiatives such as the ClimateRISE Alliance are fostering collaboration between government, private sector, academia, and civil society, enabling integrated climate–health action.
- Disaster Preparedness and Early Warning Systems:
- Forecasting and Risk Reduction: The India Meteorological Department provides advanced weather forecasting, heatwave alerts, and cyclone warnings, enhancing preparedness.
- Institutional Response Mechanism: The National Disaster Management Authority leads disaster risk reduction strategies, including climate-resilient infrastructure planning.
- These initiatives strengthen anticipatory governance and reduce mortality, morbidity, and economic losses during extreme events.
Global Initiatives & Best Practices

- Global Climate Governance and Temperature Targets:
- Multilateral Frameworks: The United Nations Framework Convention on Climate Change and the Paris Agreement form the core architecture of global climate governance, promoting mitigation, adaptation, and climate finance.
- 1.5°C Threshold- Public Health Imperative: There is a strong global scientific consensus that limiting global warming to 1.5°C is essential to avoid catastrophic and irreversible public health impacts, including large-scale mortality, disease expansion, and system collapse.
- This reinforces that climate targets are not just environmental goals, but critical health safeguards.
- Climate–Health Integration in Global Policy:
- WHO-Led Health-Centric Approach: The World Health Organization emphasises mainstreaming health into climate policy, advocating:
- Climate-resilient health systems
- Health-focused adaptation planning
- Capacity building in vulnerable countries
- It also stresses the need for financial and technical support to developing countries to manage climate-induced health risks and emergencies.
- Evidence, Monitoring and Data-Driven Action:
- Global Knowledge Platforms: The Lancet Countdown provides annual assessments linking climate change with health outcomes, strengthening policy accountability.
- Climate Data and Forecasting Systems: The World Meteorological Organization enables real-time climate monitoring and forecasting, supporting early warning systems and preparedness strategies worldwide.
- Climate Finance and Support Mechanisms:
- Financing Adaptation and Resilience: The Green Climate Fund provides financial assistance to developing countries for:
- Climate adaptation projects
- Resilient health infrastructure development
- Loss and Damage Mechanism: Global mechanisms such as the Loss and Damage Fund aim to support countries facing irreversible climate impacts, including health crises and disaster recovery needs.
- Climate-Resilient Health Systems and Infrastructure:
- Low-Carbon and Resilient Healthcare: A key global priority is to build health systems that are both climate-resilient and low-carbon, ensuring:
- Continuity of care during disasters
- Reduced environmental footprint of healthcare delivery
- Global Best Practices: Countries like Bangladesh have developed cyclone-resilient health infrastructure, demonstrating cost-effective adaptation models for vulnerable regions.
- Early Warning Systems and Disaster Risk Reduction:
- Technology-Driven Early Warning Success: The use of advanced early warning systems has proven highly effective in reducing mortality during heatwaves, floods, and tropical storms.
- Countries such as France and Australia have implemented heatwave alert systems, significantly lowering heat-related deaths.
- Global Replicability: These models highlight the importance of:
- Real-time alerts
- Public communication systems
- Inter-agency coordination
- Integrated Action and Co-Benefit Approach:
- Climate–Health as a Unified Policy Domain: Global best practices increasingly recognise that climate change and public health must be addressed as a single, integrated policy domain.
- Such an approach generates multiple co-benefits, including:
- Improved health outcomes
- Enhanced climate resilience
- Increased economic efficiency
- Multi-Stakeholder Collaboration: Effective models emphasise collaboration between governments, private sector, academia, and civil society, ensuring:
- Holistic policy design
- Efficient implementation and knowledge sharing
Click to Know UPSC OnlyIAS Coaching Centres
Way Forward
- Mainstreaming Health into Climate Governance: Climate policy must shift from a carbon-centric approach to a human-centric framework, where public health outcomes become the primary indicator of policy success.
- Integrating health into all climate decisions ensures holistic, people-centric, and outcome-oriented governance, rather than treating health as a secondary consequence.
- Whole-of-Society Approach: Addressing climate–health challenges requires coordinated investments from government, private sector, civil society, and international partners.
- Public–private partnerships can accelerate the development of:
- Climate-resilient healthcare infrastructure
- Innovative technologies and service delivery models
- Building Robust Local Data and Surveillance Systems: There is an urgent need to develop localised, disaggregated data systems to capture the linkages between microclimates and health outcomes.
- Strengthening digital platforms such as disease surveillance systems will enable:
- Early detection of outbreaks
- Targeted, evidence-based interventions
- Rebalancing Climate Finance: Climate finance must be rebalanced toward adaptation, particularly in the health sector, which remains underfunded.
- Governments, multilateral institutions, and philanthropy must:
- Increase funding for climate-resilient health systems
- Ensure equitable access to resources for vulnerable regions
- Promoting Community-Led and Decentralised Resilience: Community-based organisations and local governance bodies should be empowered with:
- Financial resources
- Technical capacity
- Such decentralised approaches ensure:
- Context-specific adaptation strategies
- Effective last-mile delivery of climate–health services
- Climate-Resilient and Disaster-Proof Infrastructure: Healthcare infrastructure must be designed or retrofitted to withstand extreme weather events, including:
- Floods, cyclones, and heatwaves
- This includes:
- Elevated structures in flood-prone areas
- Heat-resilient building design
- Reliable energy backup systems (e.g., solar power)
- Strengthening Preparedness and Anticipatory Governance: Expanding early warning systems, such as Heat Action Plans supported by India Meteorological Department and National Disaster Management Authority, is critical for reducing mortality and morbidity.
- Shift to Preventive Healthcare: Governance must transition from:
- Reactive → Anticipatory approaches
- Curative → Preventive healthcare systems
- This ensures long-term resilience rather than short-term crisis management.
Conclusion
The Dasra report concludes with a powerful reminder that “health is the lived experience of climate change.” Climate change is ultimately reflected in its impact on human health. India’s climate policy must prioritise saving lives and strengthening healthcare resilience, ensuring that adaptation measures promote equitable, sustainable, and health-centric development in the face of rising climate risks.
![]() 10 Apr 2026
10 Apr 2026

 It functions as a health-risk multiplier, as it intensifies pre-existing vulnerabilities such as poverty and malnutrition, accelerates disease transmission pathways, and overburdens already fragile healthcare systems.
It functions as a health-risk multiplier, as it intensifies pre-existing vulnerabilities such as poverty and malnutrition, accelerates disease transmission pathways, and overburdens already fragile healthcare systems.
 Mainstreaming climate concerns into public health planning
Mainstreaming climate concerns into public health planning Decentralised and Community-Based Healthcare Delivery:
Decentralised and Community-Based Healthcare Delivery: 
